Share
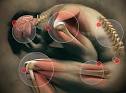 Pain is a common and disabling symptom experienced by many patients with rheumatic conditions. Neuroscientist have a deep understanding of the pain system but everyone else is lagging behind. There are complex brain and body nerve pathways that cause the body’s warning system to be activated and we experience this as pain. Symptoms often persist despite optimal medical intervention. The pain experienced by a patient is not simply directly related to tissue damage or injury. It is as a result of the combination of emotional, cognitive and sensory (peripheral nerve activation) factors.
Pain is a common and disabling symptom experienced by many patients with rheumatic conditions. Neuroscientist have a deep understanding of the pain system but everyone else is lagging behind. There are complex brain and body nerve pathways that cause the body’s warning system to be activated and we experience this as pain. Symptoms often persist despite optimal medical intervention. The pain experienced by a patient is not simply directly related to tissue damage or injury. It is as a result of the combination of emotional, cognitive and sensory (peripheral nerve activation) factors.
Neuroimaging is a powerful tool, which has been used to investigate the neural bases of pain. This method has enabled the discovery of several cortical and sub-cortical areas ( in the brain) , which are thought to be important in pain perception. The use of neuroimaging in patients with chronic pain has demonstrated considerable disruption of the normal structure and function of these brain regions.
In Osteoarthritis ( OA) , there is increasing evidence to support the role of centrally mediated factors in the generation of pain. Neuroimaging provided the *first direct evidence of central sensitisation in OA. This has implications on the optimisation of pharmacological, non-pharmacological and surgical treatment in OA.
The placebo ( and nocebo) effect has received much attention in recent years and neuroimaging has been used to investigate the underlying mechanism of this phenomenon.These studies support the involvement of frontal-limbic-brainstem network capable of driving endogenous ( the body’s own internal processes) opioid and dopamine release. These studies are driving methods to optimize treatment outcomes in clinical practice.
Treating and managing chronic pain requires a mind, brain and body approach to therapy as well as a partnership and common understanding between a person with pain and their therapist(s).
